Whether they’re running a busy emergency room or shepherding children through their annual checkups, many health care professionals share a common observation about their immigrant patients: When Immigration and Customs Enforcement (ICE) is active nearby, patients disappear. Some miss scheduled appointments while others delay seeking care.
These health care providers see firsthand how fear of deportation can affect daily life for immigrants and their family members. School, work, and social life may be disrupted as immigrants hunker down when confronting raids in their communities. When this disruption means that children don’t get vaccinations or chronic conditions go untreated, immigration enforcement becomes a public health issue.
Fortunately, local policies may counteract this pattern, say researchers at the University of California, San Francisco (UCSF) and the Immigration Policy Lab (IPL) at Stanford University. Their new study focused on San Francisco, where they did not find systematic evidence that immigrants used less health care in the aftermath of certain national political events, such as the 2016 U.S. presidential election, and local immigration enforcement events. One explanation for this may be San Francisco’s inclusive health care access program and efforts to reach out to immigrant patients, including after the 2016 presidential election, to ensure their ongoing access to care.
“This research grew out of the aftermath of the anti-immigrant policies that were enacted immediately following the 2017 U.S. presidential inauguration,” says study co-author Jaqueline Torres, a professor of epidemiology and biostatistics at UCSF. “We expected, based on prior evidence, that these could have an immediate and negative impact on public health and health care utilization for immigrants and their family members, even in Bay Area cities that have long supported sanctuary policies. We thought that drawing on data from local health systems would be a way to capture any impacts these events were having at a local level.”
Historically, ICE has avoided apprehending immigrants at health care facilities or other “sensitive locations,” but less so in recent years. And even rumors of ICE presence can lead immigrants to forgo care rather than risk encounters with law enforcement on their way there. Research has found that immigrants’ use of health care services decreases in response to events that make them feel threatened—for example, when Arizona passed wide-ranging anti-immigrant legislation in 2010 or when Alabama passed similar legislation in 2011.
So far, however, most research has focused on immigrants living in places that are either hostile or indifferent to their presence. Could this “chilling effect” on health care use look different in places with public policies that more actively support undocumented immigrants?
Consider San Francisco, which stands out for its welcoming, inclusive immigration policies. In 2006 the San Francisco Department of Public Health launched Healthy San Francisco, a program offering access to a wide range of medical services to all residents below a certain income threshold, regardless of immigration status. Among its 14,000 participants are many undocumented immigrants, since they are ineligible for the state’s health program, Medi-Cal.
As immigration enforcement increased under the Trump administration, the city took additional steps to make immigrants feel safe seeking care: for example, putting encouraging posters and other materials in clinic waiting rooms and making sure clinicians were informed when deportations were occurring nearby so that they could be prepared to support anxious patients or instruct ICE officers to leave their facilities, if necessary.
It appears that these efforts may have made a difference, according to the study, which was published in JAMA Network Open. The researchers analyzed 168,975 “clinical encounters” with 22,525 patients, focusing on a period of heightened anxiety about immigration enforcement from November 2015 to February 2018. They looked at Hispanic patients who used the Healthy San Francisco program at least once, as well as all adults who used it exclusively for their health care needs, since they were highly likely to be undocumented immigrants. They compared these groups to Hispanic and non-Hispanic patients whose health care was billed only to Medi-Cal.
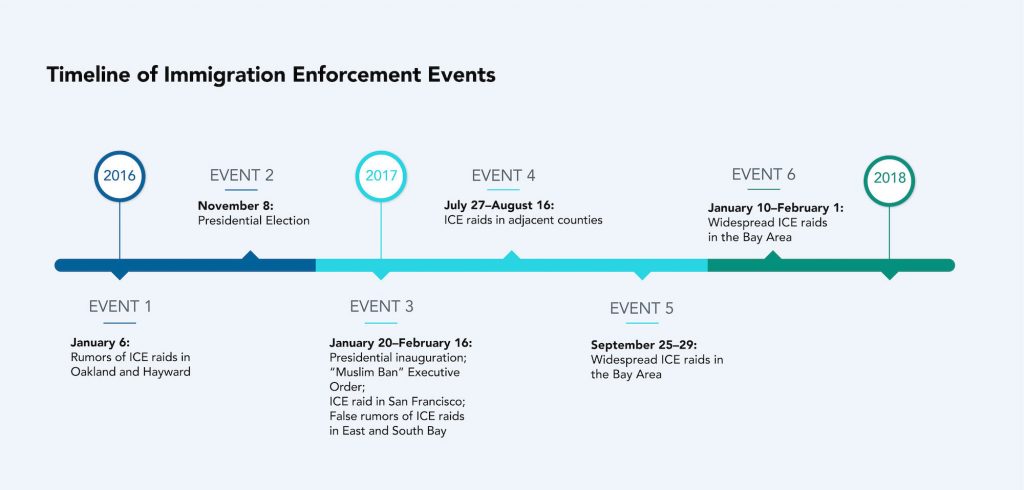
Then, the researchers picked six events that could be expected to cause fear among immigrant patients, including rumored and actual ICE raids in the Bay Area and the 2016 presidential election. They compared the five weeks before and after each event, looking at visits to primary care clinics, urgent care, and emergency departments, including parents bringing their children in for care.
Did the patients who were likely to be undocumented immigrants use less health care during times when they might be experiencing greater fear of law enforcement? No: the data showed no significant association between these threatening events and immigrants’ use of health care.
“We were rather puzzled when we first saw the results,” says IPL data scientist Vasil Yasenov. “Given prior research and anecdotal evidence of decreased care around enforcement events, we thought our aim was to quantify by how much exactly care decreases, and for which types of visits. Instead, we saw no such effects.”
While it’s encouraging to have research suggesting that inclusive health policies may help counteract a strict enforcement agenda coming from Washington, this study alone can’t tell the full story. For one thing, it only looks at how much and when people are using health care services, not the conditions bringing them in. Clinicians want to see more research on how immigration enforcement affects their patients’ health, especially among children struggling with stress and anxiety.
And since San Francisco’s citywide health coverage is rare even among urban, progressive cities, additional studies should repeat this analysis in other places. “To fully attribute this finding to health policy inclusiveness, we are hoping researchers continue to examine the immigration enforcement-health care relationship in different settings,” says Yasenov.
This is often difficult to do, however, in large part because municipal and county health systems don’t share common databases to record health care use, which prevents an “apples to apples” comparison of different patient populations.
Still, it’s important that research is helping policymakers understand the health consequences of their decisions regarding immigration. People don’t often connect immigration to public health—in political debates about immigration, we seldom hear about how restrictive policies or increased enforcement affect the way immigrants interact with health providers. Establishing that connection is the first step toward policymaking that benefits not only immigrants but also their surrounding communities.
LOCATION
San Francisco Bay Area
RESEARCH QUESTION
How does immigration enforcement affect unauthorized immigrants’ use of health care services?
TEAM
Vasil Yasenov
Jens Hainmueller
Michael Hotard
Duncan Lawrence
Laura Gottlieb
Jacqueline Torres
RESEARCH DESIGN
Difference-in-Differences
KEY STAT
Latinos make up two thirds of participants in Healthy San Francisco